Screening for Prostate Cancer – 2021 Clinical Update for Medical Professionals
If you have any questions, to schedule a consultation, please contact us or call/text: 1-646-663-5515.
We have excellent reviews from patients and their partners. Information for out-of-state and international patients. Find out our office hours or directions to our office.
We offer affordable appointment prices with or without insurance. Same-day virtual video appointments and in-person appointments are available.
Dr. Alex Shteynshlyuger is a fellowship-trained urologic oncologist, a robotically-trained surgeon who specializes in all aspects of care for early, advanced, and metastatic prostate cancer. He is a member of the Society for Urologic Oncology as well as the American Society for Clinical Oncology.
History of Screening for Prostate Cancer

PSA test has been used as a screening test for early detection of prostate cancer starting in the late 1980s. As a screening test, PSA suffers from relatively poor specificity at values less than 10 ng/dl. This has led to overdiagnosis of low-risk prostate cancer. Randomized controlled studies have also shown decreased metastatic disease burden and improved prostate-cancer mortality among screened men (ERSPC). However, overtreatment is both costly and associated with significant morbidity.
Innovations in Prostate Cancer Screening – 2021 Perspective
With >32,000 deaths from prostate cancer per year in the US alone, early detection of disease that is destined to become metastatic and cause morbidity and death present a desirable goal. The goal is to balance the risks of overdiagnosis and overtreatment of less aggressive disease that may never become clinically relevant to the benefits of early detection of aggressive disease.
Approaches to Improve Detection of High-Risk Prostate Cancer and Minimize Overdiagnosis / Overtreatment
The search for a perfect screening test is still on to replace the PSA test. Several promising approaches are available. One is to use a better screening test. Here we have a few tests to choose from: PHI (prostate health index) test has improved the ability to separate men with elevated PSA into those who are more likely to have prostate cancer from those who are more likely to have benign disease. PHI test can prevent unnecessary biopsies, but it only offers incrementally better information compared to the PSA test alone.
The 4KScore test is designed to separate men with a high risk for aggressive prostate cancer from those with no prostate cancer and low-risk prostate cancer.
Another option is to choose men with a higher risk for aggressive disease by stratifying lower Gleason biopsy results using molecular and genetic markers.
Prostate MRI is another tool that can be used to detect higher-risk prostate cancer and to select men for targeted prostate biopsy.
Where to Get Screening and Testing for Prostate Cancer in NYC?
At New York Urology Specialists, we offer treatment for men with abnormal PSA and prostate cancer. Same-day virtual video appointments and in-person appointments are available.
Call/text today: 1-646-663-5515 or make an appointment online.
We perform procedures such as prostate biopsy, transrectal prostate ultrasound, hydrogel insertion prior to radiation therapy (SpaceOAR), prostate surgery, prostate enucleation for enlarged prostate, and Urolift procedure. We treat prostate cancer, urinary problems, and erection problems and offer comprehensive STD testing for infections. We offer confidential appointments.
Our appointment costs are affordable with or without insurance. We offer free insurance verification.
Molecular and Genetic Approaches to Patient Stratification
A number of molecular and genetic markers have been identified that predict a higher risk of high-risk prostate cancer. Screening for prostate cancer with tests that have higher specificity for high-risk prostate cancer holds the promise of curing men with clinically significant disease (that is likely to become metastatic and cause death) while avoiding overtreatment.
A number of genetic mutations, including ERG and PTEN have been identified that put men at higher risk for metastatic disease and death. A number of commercial tests, including PersonalizedDx FISH test for ERG+ and PTEN aim to improve prognostication for men diagnosed with prostate cancer. This will allow us to better select men for active surveillance who are low risk and those at higher risk for active treatment.
Surgical Treatment of Prostate Cancer
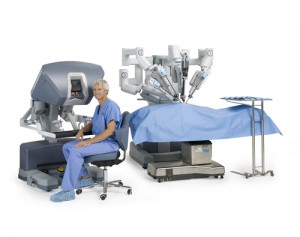
The interim upgrade of the DaVinci Robotic system to DaVinci Xi is a step toward utilization of the robotic system in more exquisite situations requiring advanced manipulation and access such as metastasectomy and extended lymph node dissections.
Conclusion
Improved sensitivity of screening tests for high-risk disease allows us to detect high-risk cancer while avoiding the problem that plagued PSA as a screening test, namely overdiagnosis. 4KScore appears to be most promising in this regard, with PHI being useful as well. Combined with genetic profiling of prostate biopsies, our new tools allow us to only select men who are at high risk for symptomatic disease for treatment while allowing a safer approach to active surveillance for men who are at low risk of experiencing morbidity of prostate cancer.
Improved efficacy of treatment, such as Zytiga, Xtandi, Xofigo, and Provenge that lead to improved overall survival in RCTs (randomized controlled trials) provide further rationale for high-impact screening for high-risk prostate cancer.
Did you know? Dr. Shteynshlyuger has performed over 1,000 prostate, penile, and bladder surgeries, including prostate biopsy, prostate removal, penile implants, Urolift, prostate enucleation, correction of Peyronie’s disease, and MRI fusion biopsy.
Cost of Prostate Cancer Treatment without Insurance
At New York Urology Specialists, we offer affordable treatment for men. Our prices are low for patients without insurance and for those who have high insurance copays, high deductibles, or insurance plans that do not cover treatment costs.
At New York Urology Specialists, we offer flat-fee ‘all-cost-included’ procedures such as prostate biopsy, hydrogel SpaceOAR insertion, circumcision, no-scalpel vasectomy, testicular implant, vasectomy reversal, hydrocelectomy, varicocelectomy, and many more. The procedures are performed in our office under local anesthesia or sedation. Men from other states can save thousands of dollars over local hospital fees by coming to New York Urology Specialists for treatment. Please contact us for current prices and discounts for patients without insurance or with high insurance deductibles.
Cost of Prostate Cancer Treatment and Insurances

We accept many health insurance plans. We would be happy to verify your eligibility and benefits and provide you with detailed information on your health plan’s coverage. Financing options and credit options are available to help you pay for medical care.
Why Choose New York Urology Specialists for Prostate Cancer Treatment?
- All treatment is performed by a board-certified urologist experienced in treating men with rising PSA, prostate cancer, enlarged prostate, erectile dysfunction, low testosterone, scrotal and testicular problems, and urinary problems using medical therapy, minimally invasive therapies, lasers, and surgery.
- We are one of the few practices in the region to offer a full range of options for the treatment of sexual, urinary, and erection problems in men.
- We offer treatment options for side effects and complications of prostate cancer treatment including erectile dysfunction, Peyronie’s disease, urinary problems, frequent urination, and overactive bladder in our office. Office procedures avoid the risks, costs, and recovery from general anesthesia.
- We offer diagnostic testing in our office, which avoids hospital costs.
- Extensive experience: Thousands of men have been treated successfully for elevated PSA, prostate cancer, erection problems, and urinary incontinence.
- Confidential and Understanding Care. We understand that most of our patients desire privacy. We see patients with a variety of urological problems. Your reason for visiting us is entirely confidential.
- We are conveniently located within a 30-60 minute commute to men who are seeking treatment for testicular and penile problems, erectile dysfunction, enlarged prostate, urinary, and cancer treatment in Manhattan, Brooklyn, Queens, Staten Island, Westchester, Long Island, Bronx, and New Jersey.
What do Prostate Cancer Problems Look Like?
You can find pictures of Prostate Cancer as well as before and after treatment images in our image gallery.
Scheduling Appointments for Prostate Cancer Treatment at New York Urology Specialists
If you have any questions, to schedule a consultation, please contact us or call/text: 1-646-663-5515.
We have excellent reviews from patients and their partners. Information for out-of-state and international patients. Find out our office hours or directions to our office.
We offer affordable appointment prices with or without insurance. Same-day virtual video appointments and in-person appointments are available.
Dr. Shteynshlyuger MD is a board-certified urologist in NYC who specializes in treating men with elevated PSA, prostate cancer, sexual, testicular, hormonal, urinary, and sexual problems in men. He has performed hundreds of penile and prostate surgeries, including penile implants, surgery for enlarged prostate, and many other procedures.
by Winston - via Healthgrades.com on Feb 14, 2021
Dr Alex Shteynshlyuger is the best urology doctor there is. He is attentive, analytical, knowledgeable and skillful. Very confidential with a masterfully professional staff. I would not hesitate in recommending Dr Shteynshlyuger to the world because I am a satisfied patient of his.
by via HealthGrades.com on Jan 29, 2021
Dr. Shteynshlyuger helped to solve my problem with ED
by A. Pereira via Vitals.com on Jan 21, 2021
Very Pleased, I couldn’t have asked for more from Dr. S as well as everyone in the office, The procedure and after was a dream with Dr. S. If you are on the fence, I can tell you, that you will love your experience with Dr. S
by Vladimir via Google.com on Sep 23, 2020
I have been observed by Dr. Alex for many years and I must say that he is a highly qualified diagnostician, and also several times I have received qualified microsurgical assistance and very useful advice. The only reason I put 4 with a plus is a somewhat long wait for the reception.
by Grant via Google.com on Aug 20, 2020
To Dr. Shteynshlyuger and your assistants and aids, thank you guys for a successful procedure. I'd refer you to others for your compassionate, knowledgeable, attentive service and indepth follow up care.
by via HealthGrades.com on Apr 12, 2020
excellent doctor and all very friendly staff
by Christopher via Google.com on Mar 11, 2020
The staff is very professional. Doctor Shteynshlyuger provided me with the care I needed. The wait, visits, and instructions were brief. I followed his instructions and my issue was resolved. As a patient exercise patience. Follow the instructions and be honest about your condition and what you hope to accomplish be visiting. Thanks again Doctor.
by JOHN on Jul 18, 2019
Therefore I would like to recommend you to anyone who need your services.
by Oliver on Jul 18, 2019
Staff were all very welcoming. Dr. Alex Shteynshlyuger was very knowledgeable and attentive during my time spent with him.
by HealthGrades.com on Jun 18, 2019
Dr. Shteynshlyuger is a very patient, understanding and caring doctor. I came to take opinion on my father’s treatment going on in my home country. Highly satisfied from his responses. He even responded to so many of my queries through patient portal . Highly grateful.
by DAM BEN STANTON on Sep 24, 2018
From the very appointment to the last follow-up visit, I felt I was at the right place and with the right people around me. Dr. Alex Stheynshlyuger and his staff made it easy and confortable. I would recommend them to every man.
by Wyts on Sep 15, 2018
Wyts Wyts recommends New York Urology Specialists via Facebook. September 15, 2018 · Friendly , courteous, effiecient and professional staff members. This office i highly recommend for any and all Urology matters. Dr Alex Shteynshlyuger is very professional and knowledgable easy to communicate with. Thanks Dr Alex
by Winston on Sep 15, 2018
I am very please and satisfied with everything that has been offorded to me by New York Urology Specialist Office.....Dr Alex
by Lee St. James on Sep 01, 2018
Dr Alex and his staff are through professionals in every sense of the word. From initial diagnosis to a period of evaluating and ruling out options, we decided upon a surgical solution, which appears for the most part to have corrected the issue. Thanks to Ana, and the staff, especially Dr. Alex for treating me so well. Best regards, Lee
by juanito creque on Apr 11, 2018
I am very satisfied with the treatment I received at new york urology specialist and would recommend them to other patients.they are the very best.
by Bob Brown on Nov 19, 2017
I am writing to thank dr. Alex. He is thorough, professional, knowledgeable, helpful and friendly. I have seen him for ED and prostate issues, and he has explained all my options clearly, and found solutions that have been a great help. thank you! I highly recommend both Dr. Alex and his staff, which I find to be helpful, friendly, knowledgeable and very professional. They are a pleasure to deal with and all have been a great help.
by Clarence Brown on Sep 14, 2017
I am very much thankful for meeting Dr Alex .I had a very serious medical problem I visited many doctors but none could not help me it was very difficult for me until I visited Dr Alex after a couple visits my medical problem is no more I feel very great also I felt almost 20 years younger Dr Alex is second to none fantastic doctor. Thanks again Dr Alex from my family.
by Michael on Jul 03, 2014
I am feeling better now after visiting clinic New York urology specialists. Excellent staff and appointment on time.
by John & Pat on May 16, 2013
Dear Dr. Alex -On behalf of John and myself – Our thanks to you for the care and concern of your help to Jack with his cancer problems. We will miss you & wish you only the best. Sincerely John & Pat Date: 2013
by George & Sally R on Jan 07, 2013
Dear Dr. Alex: We want to thank you for the excellent care you provided for George during his emergency operation and the follow up treatment. Your quiet, confident manner was reassuring to us during a very scary time for us. We will never forget you. George Sally R. Date: 2013
by Joanne R. on Sep 17, 2012
Dear Dr. Alex – I just wanted to write you a note to thank you for all of the care you have gave to my father during his illness. We appreciate all that you did to help my dad through his illness. We wanted to be sure to let you know how much it meant to us. Sincerely Joanne R.
by Joyce T on Feb 16, 2012
Dr. Alex Shteynshlyuger and Staff – Thank you so much for taking care of my husband Bob. Dr. Alex: I thank God everyday for you. You were an answer to prayer.
Treatment for Men With Fast Recovery at New York Urology Specialists

Urologists are doctors specializing in the treatment of men with prostate cancer, urinary, and sexual problems that include penis problems, scrotal problems, and erectile dysfunction. By virtue of our experience and skill, we are able to offer an effective treatment option for nearly every man who desires an effective treatment for any problem that affects the penis. We offer medical and surgical treatment for men’s sexual problems.
We Treat Some of the Most Complex Men’s Health Problems:
- Erectile dysfunction in men for whom Viagra and Cialis do not work.
- Enlarged prostate
- Penile Pain During Sex
- Impotence in men with diabetes.
- Premature Ejaculation
- Peyronie’s Disease
- Burning during urination
- Urinary retention
|
If you have any questions, to schedule a consultation, please contact us or call/text: 1-646-663-5515.
We have excellent reviews from patients and their partners. Information for out-of-state and international patients. Find out our office hours or directions to our office.
We offer affordable appointment prices with or without insurance. Same-day virtual video appointments and in-person appointments are a






 Schedule an Appointment with Dr. Shteynshlyuger:
Schedule an Appointment with Dr. Shteynshlyuger: